Insurance Verification for Medical Practices
Eligibility, benefits, and prior authorization handled by trained medical VAs — with automated checks that catch payer discrepancies before they turn into denied claims. Your billing team sees fewer denials; your patients get clear cost expectations before they arrive.
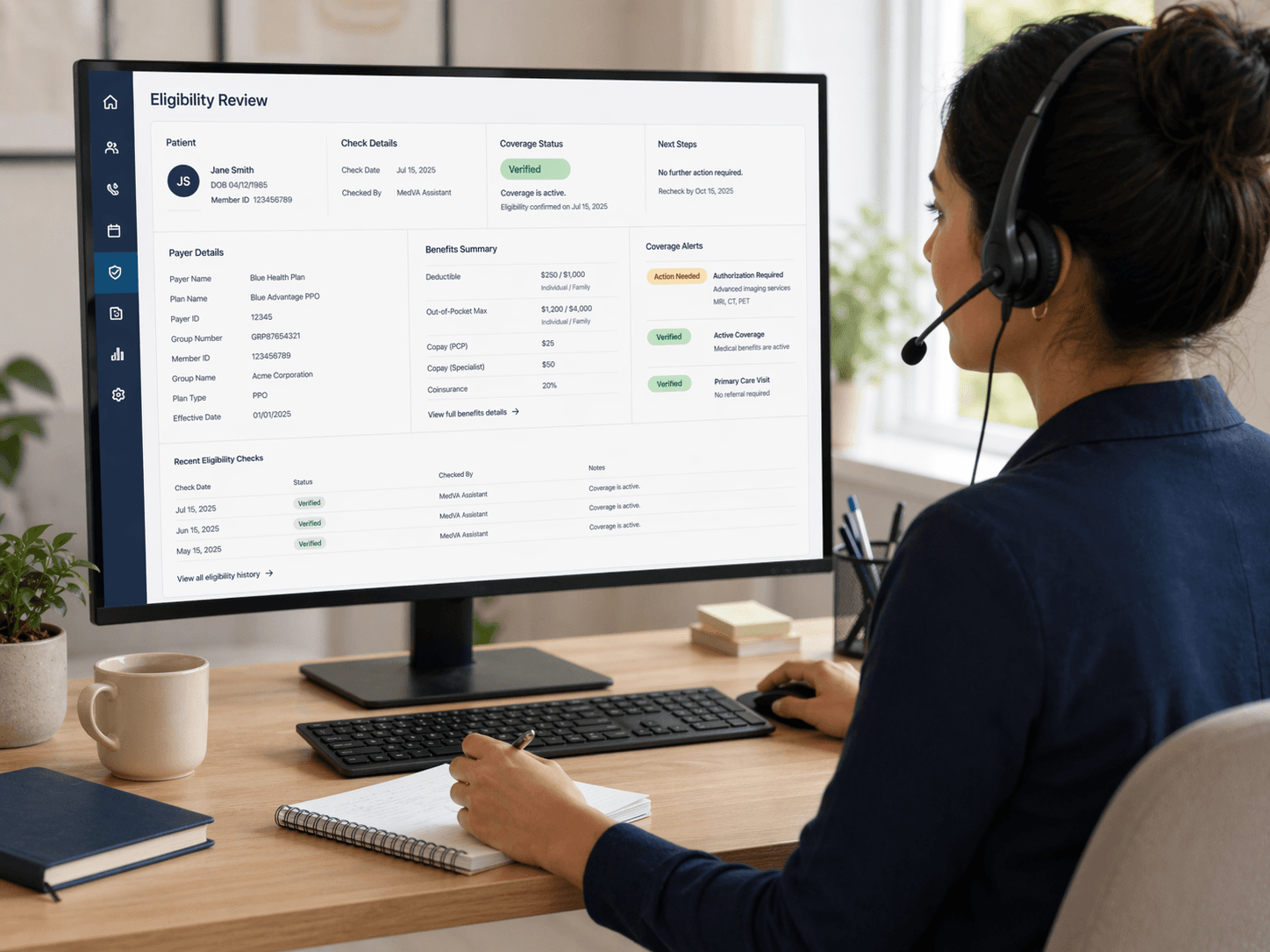
What Our Insurance Verification Service Covers
Six recurring verification lanes a trained medical VA owns end-to-end before each visit.
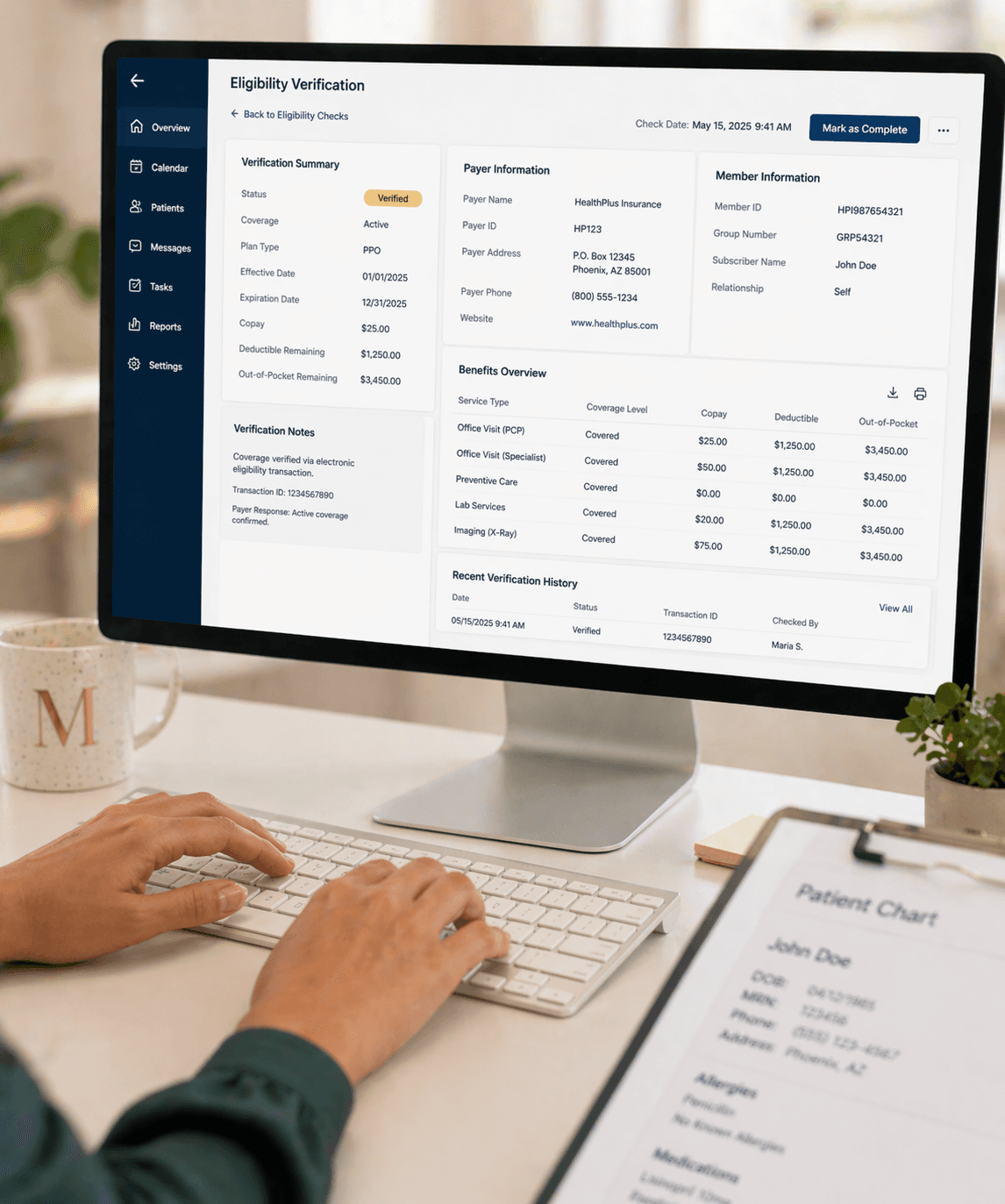
Tooling runs the first pass on eligibility and coverage; a trained medical VA reviews every flag, calls payers for anything unclear, and routes clean documentation to your billing team.
- Real-Time Eligibility
- Benefits Investigation
- Prior Authorization
- Patient Cost Estimates
- Payer Discrepancy Flagging
- Claims Follow-Up Hand-Off
Benefits of Hiring a Verification Team
Clinics that move insurance verification to a dedicated, process-driven team consistently see denials drop, prior-auth turnaround shrink, and front-desk financial conversations get shorter.
Fewer Claim Denials
Coverage issues get caught before the visit, not at adjudication — so denials driven by eligibility or missing auth decline measurably.
Faster Prior Authorization
Structured tracking and deliberate follow-up cut the turnaround time on auths that usually stall for days.
Clear Patient Estimates
Patients arrive knowing what they owe. Fewer surprise bills means fewer angry calls after the fact.
Reduced Billing Rework
Clean payer data at the front end means the billing team isn’t re-opening charts weeks later to rebuild claims.
Better Check-In Conversations
Front desk has accurate coverage info in hand, so every financial conversation is factual and short.
Consistent Payer Data
Every verification follows the same SOP, so your EHR and billing system see the same fields filled in the same way.
Secure, HIPAA-Compliant Verification Workflows
Every verification workflow runs through HIPAA-trained medical VAs operating in monitored environments with strict security protocols. Payer access, PHI handling, and documentation all follow documented procedures that are reviewable on demand. Verification decisions are logged, so billing teams and auditors see the full trail from eligibility lookup to final disposition.
We sign a Business Associate Agreement (BAA) with every practice we support.
Insurance Verification FAQs
Do you verify before every visit, or just new patients?+
What payers do you work with?+
How do you hand off to our billing team?+
Can you handle prior authorizations end-to-end?+
Speak to a Remote Medical Staffing Expert
Share your current denial rate and prior-auth backlog. We’ll scope a verification team that fits the volume.
Connect
Book a 20-minute consultation. We review your payer mix, current workflow, and denial patterns, then outline a phased rollout.
Book a ConsultationCompliance First
HIPAA-trained VAs, signed BAA, role-based EHR access, and auditable workflows on every PHI touch.
Learn about our standards